From screening to diagnosis to treatment, we’re changing everything about prostate cancer.
When you hear “it’s prostate cancer,” you may feel like everything changes.
Smarter screening
Most prostate tumors grow slowly and don’t spread. But some can spread unless you stop them early — even before you have symptoms.
- Age 50-55 for most men.
- Age 40-45 for men at higher risk of getting prostate cancer. This includes men with African ancestry, certain genetic mutations or a family history of some cancers.
The IsoPSA test detects changes in PSA molecules instead of just measuring how much PSA is in your blood. That means the test is better at informing patients and their urologists if a prostate biopsy is needed.
Many men who used to be recommended for a biopsy after their PSA test may no longer need one. In fact, one study found that prostate biopsies recommended on the basis of PSA alone were avoided in 50% of men who had the IsoPSA test.
Cleveland Clinic became the first medical center to offer the IsoPSA test to patients in 2020.
More effective monitoring
Active surveillance allows you to delay — and maybe even avoid — treatments like surgery and radiation, which can cause urinary, sexual and rectal side effects.
The strategy is safe and effective for patients with low-risk, slow-growing tumors. To better identify these patients, Cleveland Clinic helped develop the Oncotype DX® Genomic Prostate Score. This test evaluates genes in prostate tumor cells. These genes can indicate how aggressive a cancer tumor is.
This genomic test can be done on the same tissue used for your biopsy. It can predict how likely your cancer is to spread even 20 years from now. Better understanding your individual risk reveals whether you need treatment right away or just active surveillance.
Download our free prostate cancer treatment guide
One in eight men will receive a prostate cancer diagnosis during his lifetime. In its early stages, the disease rarely causes symptoms, but you may experience certain warning signs as it progresses. Here’s what to be on the lookout for.
Better biopsies
A biopsy is when your doctor takes cells from your prostate to be examined in a lab. Studying these cells under a microscope is the only way to diagnose prostate cancer.
Focal One® High-Intensity Focused Ultrasound
Specialized therapies
If your prostate cancer needs more than monitoring, Cleveland Clinic offers the most innovative treatments. In addition to standard surgery, brachytherapy and radiation therapy, we treat prostate cancer with breakthrough therapies, such as:
Focal One® high-intensity focused ultrasound. This procedure uses high-intensity sound waves to destroy cancer tumors in patients with low-risk disease. It’s delivered through a rectal ultrasound probe. There are no incisions. Most patients need no pain medication after treatment. And there are fewer side effects than with radiation therapy or prostate removal.
Lorem ipsum dolor sit amet, consectetur adipisicing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in.
Lorem ipsum dolor sit amet, consectetur adipiscing elit
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore.
Risus commodo viverra maecenas accumsan lacus vel facilisis. Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua.
Lorem ipsum dolor sit amet, consectetur adipiscing elit
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore.
Risus commodo viverra maecenas accumsan lacus vel facilisis. Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua.
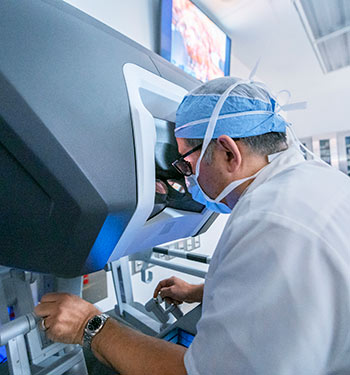
Innovative Surgical Techniques
- Outpatient prostate removal. Cleveland Clinic was the first in the U.S. to remove a patient’s prostate robotically through a single incision. Most patients having this single-port robotic procedure go home a few hours after surgery. Recovery time is shorter than with standard prostate removal. Most patients feel fine with over-the-counter pain medication or none at all. While not all patients can have single-port robotic surgery, even those who have prostate removal by standard techniques typically go home the same or next day.
- Partial prostate removal. This new type of surgery removes only the part of the prostate that has the cancer tumor. By leaving the healthy part in place, patients have fewer urinary and sexual symptoms than with standard prostate removal. This procedure is so new that there are no long-term studies on how effectively it controls prostate cancer, but early results are promising in select patients.
Virtual Second Opinions connect you online with top Cleveland Clinic specialists who can review your diagnosis and offer additional consultation quickly and securely.
Virtual Second Opinions
You can connect with Cleveland Clinic specialists from any location in the world via phone, tablet or computer, eliminating the burden of travel time and other obstacles.
You can use a Virtual Second Opinion to:
- Make the most informed decision about your healthcare or that of a loved one.
- Ensure your diagnosis is correct.
- Ensure your treatment plan is optimal for you.
- Get peace of mind and confidence that you are pursuing the best possible outcome.
Lorem ipsum dolor sit amet, consectetur adipisicing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in.
You're invited!
Join our free online health talks with urology experts from Cleveland Clinic. From urologic cancers and survivorship after treatment to erectile dysfunction and overactive bladder, our experts are here to help.
Sign up to receive invitations to upcoming online health talks!





